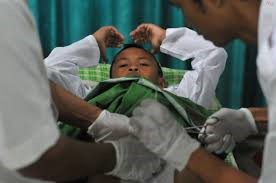
Child circumcision the surgical removal of the foreskin from the penis remains one of the most widely practiced procedures globally. Performed for religious, cultural, and medical reasons, the practice continues to generate discussion among healthcare professionals and policymakers regarding its benefits, risks, and ethical implications.
A Practice Rooted in Tradition
Circumcision is deeply embedded in the traditions of several religious and cultural groups. In Judaism and Islam, it is considered a significant rite of passage, often carried out in infancy or early childhood. In parts of Africa and other regions, the procedure is also practiced as a cultural marker of identity, transition into manhood, or social belonging.
In countries such as Nigeria, circumcision is commonly performed shortly after birth, often in hospitals or clinics, though traditional settings are still used in some communities.
Medical Perspective and Health Benefits
From a medical standpoint, child circumcision has been associated with certain health benefits. According to global health authorities such as the World Health Organization, male circumcision can reduce the risk of heterosexual transmission of HIV in high-prevalence regions. It is also linked to a lower risk of urinary tract infections in infancy and a reduced likelihood of some sexually transmitted infections later in life.
Some studies suggest that circumcision may decrease the risk of penile cancer, though the condition is already rare. Additionally, it can prevent foreskin-related conditions such as phimosis, where the foreskin cannot be fully retracted.
Risks and Medical Concerns
While generally considered a safe procedure when performed by trained professionals in sterile environments, circumcision is not without risks. Possible complications include bleeding, infection, and improper healing. In rare cases, more serious complications can occur, particularly when the procedure is carried out in non-clinical settings without adequate hygiene or medical expertise.
Health professionals emphasize the importance of proper surgical standards, pain management, and post-procedure care to minimize these risks.
Ethical Debate and Consent
Beyond medical considerations, child circumcision raises ethical questions, particularly around consent. Critics argue that performing an irreversible procedure on infants or young children who are unable to make informed decisions may infringe on bodily autonomy.
Human rights organizations, including groups such as Amnesty International, have at times highlighted concerns about non-therapeutic circumcision performed without the individual’s consent. Advocates of the practice, however, maintain that parental rights, cultural traditions, and perceived health benefits justify early circumcision.
Public Health and Policy
Policies on child circumcision vary widely across countries. In some nations, it is routinely offered in hospitals, while in others, it is less common or subject to stricter regulations. Public health campaigns in parts of sub-Saharan Africa have promoted voluntary medical male circumcision as part of broader HIV prevention strategies.
Experts stress that where circumcision is practiced, ensuring safe, accessible, and regulated medical services is essential to protect children’s health.
Informed Decision-Making
Medical professionals increasingly encourage parents to make informed decisions based on accurate information, cultural values, and medical advice. Discussions with qualified healthcare providers can help families understand both the potential benefits and risks.
As global perspectives continue to evolve, child circumcision remains a complex issue at the intersection of health, culture, religion, and ethics one that requires careful consideration and respectful dialogue across diverse communities.