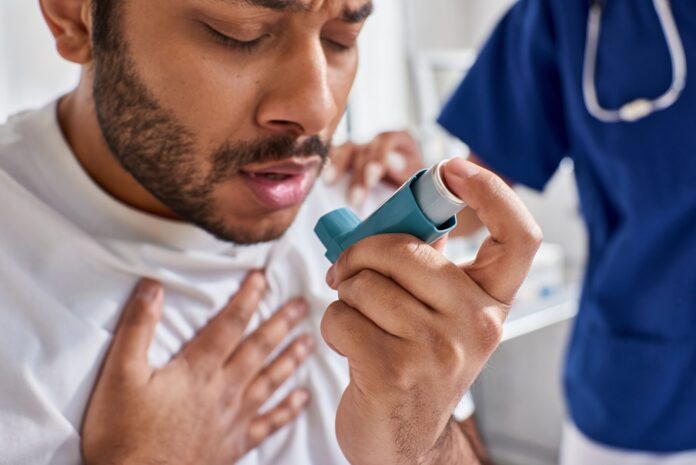
Asthma continues to disproportionately affect African American populations, with experts pointing to a complex mix of biological, environmental, and social factors driving the disparity. The chronic respiratory condition, known as Asthma, affects people of all backgrounds, yet outcomes remain significantly worse in some communities.
Higher Risk and More Severe Outcomes
Available data show that African American individuals face a higher likelihood of developing asthma compared to their white counterparts. In addition to increased prevalence, the condition often presents more severely, leading to higher rates of emergency care visits and mortality.
Health professionals note that individuals in these communities are more likely to experience frequent asthma attacks and complications, highlighting a growing public health concern.
Biological Factors Under Investigation
Researchers have identified possible biological differences that may contribute to the severity of asthma in African American populations. One area of focus is airway inflammation, particularly a form involving elevated levels of immune cells that can worsen breathing difficulties.
This type of inflammation is closely linked to more persistent and difficult-to-control asthma symptoms, even when standard treatments are used.
The Role of Genetics
Genetic factors are also being explored as a contributing element. Some studies suggest that variations in genes may influence how individuals respond to common asthma medications, including bronchodilators used to open the airways.
These differences could partly explain why some patients experience reduced effectiveness from standard treatments, making disease management more challenging.
Inequities in Healthcare Access
Beyond biology, systemic issues play a critical role. Limited access to quality healthcare services remains a major barrier in many underserved communities.
Delayed diagnosis, inconsistent treatment, and reduced access to preventive care can all contribute to poorly managed asthma and increased complications.
Environmental and Social Determinants
Environmental exposure is another significant factor. Poor housing conditions, air pollution, and exposure to allergens such as mold can increase the risk of developing asthma and trigger more frequent attacks.
Socioeconomic challenges, including low income and limited access to clean living environments, further compound the problem, making effective disease control more difficult.
Early-Life Risk Factors
Research also indicates that children born with low birth weight—more common in underserved populations—may face a higher risk of developing asthma later in life. This highlights the importance of maternal health and access to quality prenatal care.
Recognizing Symptoms and Seeking Care
Common symptoms of asthma include:
-
Wheezing
-
Shortness of breath
-
Persistent coughing
-
Chest tightness
Early diagnosis is essential. Medical evaluation typically involves lung function tests and imaging to rule out other conditions.
Treatment and Management
While treatment approaches do not differ by race, effective management is critical, particularly in high-risk populations. Standard care includes:
-
Medications such as bronchodilators and anti-inflammatory drugs
-
Identifying and avoiding triggers
-
Regular monitoring and follow-up care
Lifestyle adjustments, including avoiding smoking and maintaining a healthy environment, also play a key role in controlling symptoms.
Prevention and Public Health Response
Experts emphasize that reducing asthma disparities will require coordinated public health efforts. Key strategies include:
-
Expanding access to affordable healthcare
-
Improving housing and environmental conditions
-
Strengthening community health education
-
Reducing exposure to air pollution and tobacco smoke
Policy reforms aimed at addressing systemic inequalities are also considered essential to long-term progress.
Conclusion
The higher burden of asthma in African American communities reflects a combination of medical, environmental, and societal factors. Addressing these disparities will require sustained efforts from healthcare providers, policymakers, and communities alike.
Improving access to care, advancing research, and tackling underlying inequalities remain critical steps toward reducing the impact of asthma and improving health outcomes for vulnerable populations.